Improving the diagnosis of coeliac disease
Around 1 in 100 people in the UK have coeliac disease. Having this condition means your immune system attacks the tissues in your digestive system when you eat gluten. Many people who have the condition haven’t yet been diagnosed with it. People with untreated coeliac disease have an increased risk of anaemia, osteoporosis and cancer. The only treatment available is a gluten free diet.
Diagnosing coeliac disease can be difficult. Some people may not have any symptoms, while others have non-specific symptoms such as indigestion or bloating. It’s thought only one in three people with coeliac disease are actually diagnosed.
Guidelines recommend that adults and children “at high risk” of coeliac disease should be offered testing. However, it is not clear which groups are at high enough risk to justify routine testing, which symptoms should lead to testing, which tests should be offered, and whether a biopsy (taking a small tissue sample) to confirm the diagnosis is necessary.
Project aims
This project was aimed at investigating the best testing strategy for identifying adults and children with coeliac disease. This strategy would have to be both cost-effective and acceptable to patients.
We wanted to establish who should be tested for coeliac disease, what tests should be offered, and whether a biopsy is necessary for all patients.
What we did
We searched for studies on coeliac disease testing to see if we could assess how accurate these tests were. Our team also reviewed and analysed the results of 191 studies looking at diagnostic indicators such as symptoms or risk conditions for coeliac disease.
In addition, we reviewed data from general practices. This was because we wanted to understand whether certain combinations of risk factors and symptoms could help identify people with an increased risk of having coeliac disease.
We interviewed 20 adults diagnosed with coeliac disease. We did this to improve our understanding of the patient experience.
We created an online survey to explore how confident people felt about a diagnosis given in different situations. We also conducted a second survey to assess the quality of life of people living with the disease. This survey included questions about adherence to a gluten-free diet and gave respondents space to provide additional comments .
Finally, we assessed the cost-effectiveness of different diagnostic strategies.
What we found and what this means
Blood test accuracy
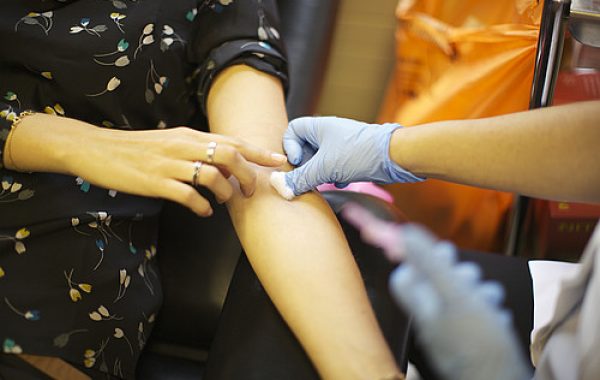
To assess the accuracy of blood tests for coeliac disease in adults and children, we looked at 113 studies. We reviewed studies comparing the results of blood tests with duodenal biopsies. Blood tests aimed at diagnosing coeliac disease look for antibodies in a person’s blood that might be associated with this disease. A duodenal biopsy involves a small section of a patient’s duodenum (the initial C-shaped segment of the small intestine) being taken so it can be examined under a microscope.
We found that the accuracy of blood tests for detecting coeliac disease was high. They are a useful first step towards diagnosis in patients suspected of having coeliac disease. Our findings suggest that blood tests alone could be used for diagnosis in some people, without the need for a biopsy.
Identifying people at risk of developing coeliac disease
During this part of the study, we identified and focused on 26 signs, symptoms and risk factors associated with coeliac disease.
We found strong evidence that people with a family history of coeliac disease, dermatitis herpetiformis (a skin condition caused by a reaction to gluten ingestion), anaemia, type 1 diabetes, migraines, certain genes, osteoporosis, or chronic liver disease are more than twice as likely to have coeliac disease than the general population. Additionally, close relatives of people with coeliac disease are three times as likely to have it themselves. These signs and symptoms could therefore help identify patients who would benefit from testing.
Migraine and chronic liver disease are not yet included as a risk factor in all guidelines. We think it may be appropriate for these to be added to guidelines.
Other signs including gastrointestinal symptoms (such as diarrhoea, constipation and abdominal pain), psoriasis, epilepsy, inflammatory bowel disease, systemic lupus erythematosus, fractures, type 2 diabetes and multiple sclerosis were not shown to be reliable indicators of the disease.
Patient experience
We found that patients experience uncertainty when following the traditional diagnostic pathway for coeliac disease. This uncertainty particularly affected patients when they wanted an explanation for their symptoms and during investigations for a potential diagnosis of coeliac disease.
Coeliac disease is traditionally diagnosed through a combination of blood tests and an endoscopic biopsy. An endoscopic biopsy involves a camera being passed into the body with a small sample of body tissue being collected so it can be examined under a microscope. One of the challenges for patients is the need to maintain a diet containing gluten in the lead up to the endoscopy.
Interviewees reported waiting a long time for an endoscopy and found it challenging to manage their diet before the procedure. However, having the procedure reassured most interviewees that they should be following a gluten-free diet for the rest of their lives. For some it increased their likelihood of adhering to the diet and reduced post-diagnostic uncertainty if their symptoms returned.
If we move toward a no biopsy approach for some patients, it is important to ensure patients receive adequate follow up and specialist support to reduce the risk of a misdiagnosis. Any uncertainty patients experience during the diagnostic process must also be addressed.
BJGP podcast about patient experience
Dr Alice Harper, an NIHR Academic Clinical Fellow based at the Centre for Academic Primary Care at the University of Bristol spoke to Nada Khan for the BJGP podcast about her study on coeliac disease.
BJGP video about patient experience
Watch the videos from Dr Alice Harper’s BJGP podcast about patient experience during disease diagnosis.
Developing prediction models
We reviewed data from general practices to see whether we could develop diagnostic prediction models to help decide who should be offered testing for coeliac disease in GP practices. Diagnostic prediction modelling uses statistics to predict whether someone has a certain condition. In this case we wanted to see whether we could predict how likely someone would be to have coeliac disease based on other conditions they may have or things we might know about them.
Our prediction model included conditions and factors that might mean either an adult or a child might have coeliac disease. Type 1 diabetes, Turner syndrome, IgA deficiency or having a close relative with coeliac disease were the strongest predictors that a child would be likely to have the disease. Anaemia and having a close relative with the disease were predictors for adults.
Although these types of models could be used by GPs to help identify people with an increased risk of coeliac disease, it would involve offering blood tests to more people than is currently done. Overall, we found that our model tended to overestimate coeliac disease risk in both adults and children.
Confidence in diagnosis and following a gluten-free diet
We organised focus groups and an online survey to find out how confident people needed to feel about their diagnosis before they started a gluten-free diet or underwent a biopsy and understanding what factors influenced their attitude. We also included questions about quality of life among people with coeliac disease and the difficulties they may face when following a gluten-free diet.
Four hundred and seventy-two people completed our survey. We found that the level of certainty people wanted varied a lot. In scenarios where we asked respondents to imagine that they had no symptoms, they wanted a higher level of certainty before committing to a lifelong gluten-free diet then when they imagined having debilitating symptoms.
Instead of starting a gluten-free diet immediately, a higher number of our respondents opted to wait for a confirmation biopsy, when given the option. This was the case even if a hypothetical blood test gave them 75–90 per cent certainty they had the disease.
Quality of life survey
Our survey showed that some people experienced coeliac disease and the associated diet as a heavy burden. Patients who worried about their health were concerned about the consequences of a late diagnosis. This suggests that delays in getting a diagnosis are associated with lower quality of life.
Those who found it hard to follow a gluten-free diet and those who were very strict about following it also had a lower quality of life. Free-text comments suggested that people adhering very strictly to a gluten-free diet may have been doing so because they experienced symptoms with minimal gluten exposure. On the other hand, people who found following a diet difficult may only recently have started following it and were still adjusting to its impact.
People struggled with the lack of awareness among friends and family, healthcare professionals, and hospitality staff and were unsatisfied with the availability and costs of gluten-free products. This means that education and improving general awareness may increase quality of life and is necessary to prevent accidental exposure to gluten, which would reduce anxiety and restrictions related to eating out.
In line with previous research, the survey highlighted the challenge of consistent follow-up care for individuals with coeliac disease. While regular follow-up is considered a vital component of patient care, in practice, follow-up care is often inconsistent or absent.
Assessing how cost-effective diagnostic strategies are
We found that the immunoglobulin A tissue transglutaminase test, currently the most common blood test for coeliac disease, was the most cost-effective at diagnosing the disease in adults, when using blood tests alone. However, using specific blood test combinations was similarly cost-effective and could be the most practical strategy for the NHS to implement (a combination of human leucocyte antigen and immunoglobulin A tissue transglutaminase testing).
What next?
We expect the results of this study to change the way people with coeliac disease are identified in the UK.
Papers

Accuracy of potential diagnostic indicators for coeliac disease: a systematic review protocol
Read the paper
Systematic review with meta-analysis: the accuracy of serological tests to support the diagnosis of coeliac disease
Read the paper
The accuracy of diagnostic indicators for coeliac disease: A systematic review and meta-analysis
Read the paper
Development and external validation of a clinical prediction model to aid coeliac disease diagnosis in primary care: An observational study
Read the paper
Defining the optimum strategy for identifying adults and children with coeliac disease: systematic review and economic modelling
Read the paper
Understanding the patient experience of coeliac disease diagnosis: a qualitative interview study
Read the paper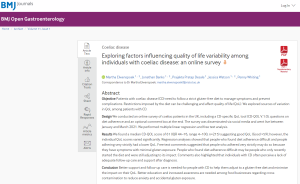
Exploring factors influencing quality of life variability among individuals with coeliac disease: an online survey
Read the paperRelated research
This project builds on this previous work.
Lead collaborators
- Dr Penny Whiting, University of Bristol
- Dr Peter Gillett, Royal Hospital for Sick Children
- Dr Gerry Robins, York Teaching Hospital NHS Foundation Trust
- Dr Hazel Everitt, University of Southampton
- Dr Hayley Jones, University of Bristol
- Dr Howard Thom, University of Bristol
- Professor Alastair Hay, University of Bristol
- Deborah Lane, Patient representative
- Jo Stubbs, Patient representative
- Dr Alice Harper, University of Bristol
- Rachel O'Donnell, University of Bristol
ARC West Staff
Dr Jessica Watson
GP and Doctoral Research FellowPartners on this project
University of Bristol
The University of Bristol is internationally renowned and one of the very best in the UK, due to its outstanding teaching and research, its superb facilities and highly talented students and staff. Its students thrive in a rich academic environment which is informed by world-leading research. It hosts the Elizabeth Blackwell Institute for Health Research.