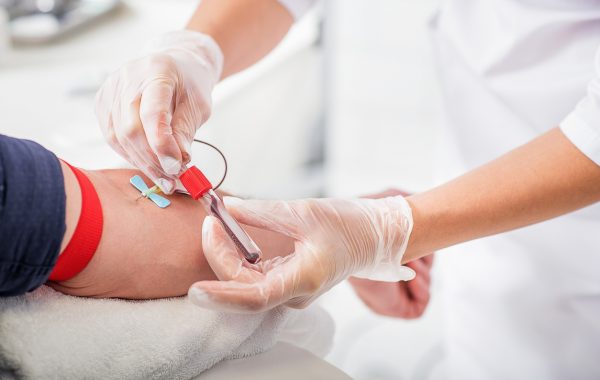
Developing recommendations for chronic disease testing in GP practices
Laboratory tests are on the rise in UK healthcare. Half of the tests ordered by GP practices are to monitor long-term conditions such as high blood pressure, diabetes and chronic kidney disease. There are guidelines on which tests people with chronic diseases should receive and how often they should be tested, but we wanted to investigate what evidence underpins them.
There is also a lot of variation in the tests GP practices order. For example, when researchers asked 20 GP practices in North Devon which tests they ordered for these patients and how often, no two practices were the same.
Testing is generally considered to be a good thing, but unnecessary tests can cause problems, such as false alarms. If test results are abnormal, further tests or referrals might be needed to find out what’s wrong. This can be worrying for patients, and sometimes doctors may never find a cause for an abnormal blood test.
Unnecessary testing can also lead to over-diagnosis, where a condition is diagnosed that would never have caused problems during a patient’s lifetime. Unnecessary testing also impacts GP workload, as the results need to be reviewed and abnormal results must be investigated. On the other hand, failure to test may lead to missed diagnoses, complications, patient harm and legal action.
Project aims
This project aims to develop evidence for recommendations on the tests people with high blood pressure, diabetes and chronic kidney disease should have to monitor their condition, and how regularly they should be tested.
What we did
We reviewed the national guidelines and the recommendations they make.
When reviewing the existing guidance, we looked at the guidelines from the National Institute for Health and Care Excellence (NICE), the Scottish Intercollegiate Guidelines Network (SIGN), the Royal Colleges of Pathologists, Physicians and General Practitioners. We also looked at ClinicalTrials.gov, which lists international clinical trials, to see if any studies on this topic were in the pipeline.
We reviewed studies that have already been done on this topic and the methods that were used as part of a ‘scoping review’. A scoping review is a new approach for mapping research evidence across broad topics. The scoping review aimed to give an overview of the studies investigating optimal testing and to examine how they went about it. We looked at what methods the researchers used to answer the questions ‘which test should GPs use and how often’ for patients with long-term conditions.
We looked at the anonymised health records of people registered with a UK GP between June 2013 and May 2018. We then reviewed the records of patients diagnosed with high blood pressure, type 2 diabetes or chronic kidney disease. We looked at the number of blood tests these patients had had during that time. We reviewed the results of over 27 million tests for nearly 1 million patients. If the data was available, we also included a patient’s age, sex, ethnicity and socioeconomic deprivation when looking at testing rates. We compared the number of tests ordered between practices as well as comparing testing rates to current guidelines for people with long-term conditions.
We surveyed GPs to understand their perspectives on using tests for monitoring long-term conditions, the workload involved in testing, and their confidence in ordering and interpreting tests results.
We also discussed the project with our health systems panel, made up of members of the public, to understand their thoughts on testing for chronic conditions.
What we found and what this means
We found that the existing guidelines used by GPs to monitor chronic conditions are based on expert opinion rather than evidence, because there is little research on this issue.
Guidelines often didn’t include recommendations on the frequency of testing, and where evidence was available, it did not address the fundamental question of whether the test was necessary or beneficial.
Our scoping review included 94 studies. We found that studies focused on which test to use but not how often the test should be repeated. Many studies investigated the accuracy of the test or compared one test to another without answering the more fundamental question whether doing the test is necessary or beneficial.
This lack of evidence for how often tests should be carried out means patients could be receiving tests unnecessarily.
Future studies need to address these gaps using strong study designs such as randomised controlled trials where the benefits to patients of one testing strategy can be compared to another.
When looking at the anonymised health records of people registered with a UK GP between June 2013 and May 2018, we found that testing rates are no longer increasing, but they don’t always follow guidelines for monitoring long-term conditions. We found that kidney function, liver function and full blood counts (a test to check the types and numbers of cells in someone’s blood) were being tested most often.
Our researchers also established that some tests weren’t being carried out as often as guidelines suggested, while others were being carried out more often. The number of tests also varied considerably between GP practices. This could mean that there is uncertainty about the most appropriate testing frequencies for different conditions.
The UK-wide GP survey was completed by 550 GPs. Results showed that how often GPs order tests for patients with chronic conditions, and which tests they order, varies considerably. This suggests that some tests may be unnecessary.
Because current guidelines are unclear, GPs make decisions about testing based on different reasons. This increases unnecessary testing, heightens GPs’ uncertainty in knowing how to act on abnormal test results, and leads to differences in care for patients.
The results from the health systems panel discussions showed that people generally assumed testing was reliable and never harmful. This underlines the need for healthcare professionals to have open discussions with patients so that they understand the risks associated with testing and can make informed decisions.
What next?
This project could improve consistency in how chronic conditions are monitored in GP practices. It is likely to mean fewer tests are performed, reducing the risks around over-testing.
We are also creating methods for other researchers to use to develop testing recommendations for other long-term conditions treated in GP surgeries.
Papers
What methods are being used to create an evidence base on the use of laboratory tests to monitor long-term conditions in primary care? A scoping review
Read the paper
Variation in laboratory testing for patients with long-term conditions: a longitudinal cohort study in UK primary care
Read the paperRelated research
This project led to a larger piece of work.
Links and downloads
- What is the evidence behind guideline recommendations to monitor chronic diseases in UK primary care? Martha's BJGP oral presentation
- Read the Pulse coverage of this study Wide variation in testing frequency for long-term conditions, finds GP study
Lead collaborators
- Ed Mann, Tyntesfield Medical Group
- Katharine Alsop, Nightingale Valley Practice
- Dr Penny Whiting, University of Bristol